 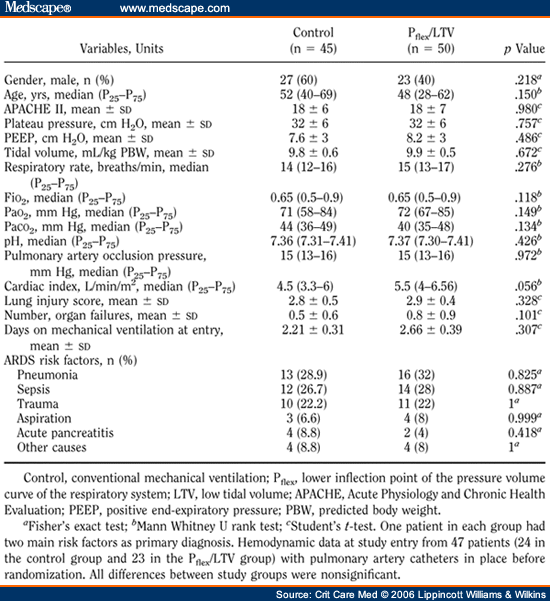
A retrospective study from Brazil showed that a low S/F at ICU admission was associated with increased risk of death in patients with severe sepsis or septic shock. Another study suggests that ARDS patients diagnosed by S/F have very similar clinical characteristics and outcomes compared with patients diagnosed by P/F. A secondary analysis of the ARDS Network trial of a lower tidal volume ventilator strategy showed that S/F correlated with P/F in patients with ARDS. Low oxygen saturation to FiO 2 ratio (S/F) within 6 h of presentation to emergency room was found to predict early development of ARDS. When coupled with the performance of point-of-care echocardiogram, the diagnosis of non-cardiogenic pulmonary edema can be achieved in acutely hypoxemic patients, including those with sepsis. 
There is a growing body of evidence suggesting that the diagnostic utility of the ultrasound exam of the lung compares well with that of the CXR. It is not clear whether the mere diagnosis of ARDS would impact care and/or outcomes of patients with sepsis or septic shock with acute respiratory failure. However, the availability (or the lack of) of CXR and ABG in resource-limited settings might preclude their timely performance and utility in diagnosing septic patient with ARDS. Therefore, in order to diagnose ARDS, performance of a chest radiograph (CXR) and arterial blood gas analysis (ABG) is necessary. The Diagnosis of the Acute Respiratory Distress Syndrome (ARDS)ĪRDS is a combined clinical and radiographic diagnosis, which per the latest consensus definition requires the presence of acute bilateral chest infiltrates (onset within less than 1 week), not primarily caused by hydrostatic pulmonary edema, associated with hypoxemia based on PaO 2 to FiO 2 ratio (P/F) of less than 300 mm Hg and requiring at least 5 cm H 2O of positive end-expiratory pressure (PEEP). “Volume-controlled” modes could be safer than “pressure-controlled” modes, and we recommend to check regularly whether a patient tolerates a “support” mode we also suggest to perform spontaneous breathing trials to timely identify patients who are ready for extubation, but also to plan extubating patients when sufficient staff is around to guarantee safe re-intubation.Ħ.2. Low tidal volumes (5–7 ml/kg predicted body weight, avoiding >10 ml/kg) are recommended and if at all possible in combination with end-tidal carbon dioxide (CO 2) monitoring for recognition of dislodgement of the endotracheal tube and under- or overventilation. Recruitment maneuvers are indicated in refractory hypoxia, but require experienced staff. In addition, low FiO 2 and low oxygenation goals are suggested, using PEEP/FiO 2 tables. These recommendations include an elevated head-of-bed position and a minimum level of positive end-expiratory pressure (PEEP) of 5 cm H 2O only to be in patients with moderate or severe ARDS. However, many of these have not been trialed specifically in resource-limited settings. A number of recommendations for safe and lung-protective mechanical ventilation in patients with sepsis and respiratory failure are provided. Bedside lung ultrasound is a valuable diagnostic tool assessing pulmonary edema and other pathologies. Where blood gas analyzers are unavailable, it can be replaced by the plethysmographic oxygen saturation/fractional inspirational oxygen concentration (SpO 2/FiO 2) gradient. 
In this chapter we discuss recommendations on the identification of patients with acute respiratory distress syndrome (ARDS), indications for mechanical ventilation, and strategies for lung-protective ventilation in resource-limited settings. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
